Abstract
Objective:
Associations between magnitude and timing of maternal pregnancy blood lead (Pb) levels (BLLs), birth weight, and total days of gestation were examined, as well as associations with related clinical diagnoses of low birth weight (LBW), preterm, and small-for-gestational-age (SGA) birth.
Study Design:
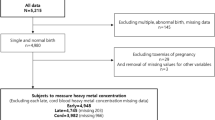
Among a sample of 262 mother–infant pairs studied retrospectively, one-way analysis of variance and regression statistics were used to measure the relationship between level of maternal pregnancy BLLs and birth outcomes while controlling for key maternal and newborn factors.
Results:
Women with maximum pregnancy BLLs (max-PBLLs) ⩾10 μg/dl tended to give birth earlier and their babies were at substantially increased risk for preterm and SGA birth. By holding other explanatory factors constant, each unit increase in max-PBLL above 10 μg/dl was found to be associated with a decrease of −0.3 in total days of gestation. Compared to women with lower levels, women with max-PBLLs ⩾10 μg/dl were at a threefold increased risk for preterm birth (adjusted OR=3.2, 95% CI 1.2–7.4) and more than a fourfold increased risk for having an SGA infant (adjusted OR=4.2, 1.3–13.9). Second trimester maximum BLLs ⩾10 μg/dl were associated with a steep decrease in total days of gestation (a decrease of −1.0 days per each unit increase above 10 μg/dl).
Conclusions:
These data provide evidence of the adverse effects of maternal pregnancy BLLs, particularly when levels are ⩾10 μg/dl. Prenatal Pb exposure at these levels was associated with significant decreases in total days of gestation and an increased risk of preterm and SGA birth.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Gardella C . Lead exposure in pregnancy: a review of the literature and argument for routine prenatal screening. Obstet Gynecol Surv 2001; 56: 231–238.
Charlton V . The small for gestational age infant. In: Rudolph A (ed). Pediatrics. Appleton and Lange: Norwalk, 1996, pp 245–248.
Gutbrod T, Wolke D, Soehne B, Ohrt B, Riegel K . Effects of gestation and birth weight on the growth and development of very low birthweight small for gestational age infants: a matched group comparison. Arch Dis Child Fetal Neonatal Ed 2000; 82: F208–F214.
Jelliffe-Pawlowski LL, Hansen RL . Neurodevelopmental outcome at 8 months and 4 years among infants born full-term small-for-gestational-age. J Perinatol 2004; 24: 505–514.
Frisbie WP, Biegler M, de Turk P, Forbes D, Pullum SG . Racial and ethnic differences in determinants of intrauterine growth retardation and other compromised birth outcomes. Am J Public Health 1997; 87: 1977–1983.
Savitz DA, Kaufman JS, Dole N, Siega-Riz AM, Thorp Jr JM, Kaczor DT . Poverty, education, race, and pregnancy outcome. Ethn Dis 2004; 14: 322–329.
Rothenberg SJ, Manalo M, Jiang J, Khan F, Cuellar R, Reyes S et al. Maternal blood lead level during pregnancy in South Central Los Angeles. Arch Environ Health 1999; 54: 151–157.
Bernard SM, McGeehin MA . Prevalence of blood lead levels > or =5 micro g/dl among US children 1–5 years of age and socioeconomic and demographic factors associated with blood lead levels 5–10 micro g/dl, Third National Health and Nutrition Examination Survey, 1988–1994. Pediatrics 2003; 112 (6 Part 1): 1308–1313.
Lin C, Kim R, Tsaih SW, Sparrow D, Hu H . Determinants of bone and blood lead levels among minorities living in the Boston area. Environ Health Perspect 2004; 112: 1147–1151.
McMichael AJ, Vimpani GV, Robertson EF, Baghurst PA, Clark PD . The Port Pirie cohort study: maternal blood lead and pregnancy outcome. J Epidemiol Commun Health 1986; 40: 18–25.
Baghurst PA, Robertson EF, Oldfield RK, King BM, McMichael AJ, Vimpani GV et al. Lead in the placenta, membranes, and umbilical cord in relation to pregnancy outcome in a lead-smelter community. Environ Health Perspect 1991; 90: 315–320.
Satin KP, Neutra RR, Guirguis G, Flessel P . Umbilical cord blood lead levels in California. Arch Environ Health 1991; 46: 167–173.
Factor-Litvak P, Graziano JH, Kline JK, Popovac D, Mehmeti A, Ahmedi G et al. A prospective study of birthweight and length of gestation in a population surrounding a lead smelter in Kosovo, Yugoslavia. Int J Epidemiol 1991; 20: 722–728.
Bellinger D, Leviton A, Rabinowitz M, Allred E, Needleman H, Schoenbaum S . Weight gain and maturity in fetuses exposed to low levels of lead. Environ Res 1991; 54: 151–158.
West WL, Knight EM, Edwards CH, Manning M, Spurlock B, James H et al. Maternal low level lead and pregnancy outcomes. J Nutr 1994; 124 (6 Suppl): 981S–986S.
Sowers M, Jannausch M, Scholl T, Li W, Kemp FW, Bogden JD . Blood lead concentrations and pregnancy outcomes. Arch Environ Health 2002; 57: 489–495.
Andrews KW, Savitz DA, Hertz-Picciotto I . Prenatal lead exposure in relation to gestational age and birth weight: a review of epidemiologic studies. Am J Ind Med 1994; 26: 13–32.
Dearth RK, Hiney JK, Srivastava V, Burdick SB, Bratton GR, Dees WL . Effects of lead (Pb) exposure during gestation and lactation on female pubertal development in the rat. Reprod Toxicol 2002; 16: 343–352.
Epstein HT, Newton JT, Fenton K . Lead effects on offspring depend on when mouse mothers were exposed to lead. Biol Neonate 1999; 75: 272–278.
Borja-Aburto VH, Hertz-Picciotto I, Rojas LM, Farias P, Rios C, Blanco J . Blood lead levels measured prospectively and risk of spontaneous abortion. Am J Epidemiol 1999; 150: 590–597.
New York State Department of Health and American College of Obstetrics and Gynecology District II. Lead Poisoning Prevention Guidelines for Prenatal Care Providers. State of New York: Department of Health: Albany, NY, 1995.
Minnesota Department of Health EHD. Blood Screening Guidelines for Pregnant Women in Minnesota. Environmental Health Division. Minnesota Department of Health: Minnesota, 2005.
Centers for Disease Control and Prevention. Screening Young Children for Lead Poisoning: Guidance for State and Local Public Health Officials. US Department of Health and Human Services: Atlanta, GA, 1997.
Centers for Disease Control and Prevention. In: Harrey B (ed). Managing Elevated Blood Lead Levels Among Young Children: Recommendations from the Advisory Committee on Childhood Lead Poisoning Prevention. US Department of Health and Human Services: Atlanta, GA, 2002.
Balcazar H . The prevalence of intrauterine growth retardation in Mexican Americans. Am J Public Health 1994; 84: 462–465.
Goldenberg RL, Cliver SP, Neggers Y, Copper RL, DuBard MD, Davis RO et al. The relationship between maternal characteristics and fetal and neonatal anthropometric measurements in women delivering at term: a summary. Acta Obstet Gynecol Scand Suppl 1997; 165: 8–13.
Olausson PM, Cnattingius S, Goldenberg RL . Determinants of poor pregnancy outcomes among teenagers in Sweden. Obstet Gynecol 1997; 89: 451–457.
Statistical Analysis Software (SAS). Version 8.0. SAS Institute Inc. Cary, NC, 1999.
Dietrich KN, Krafft KM, Bornschein RL, Hammond PB, Berger O, Succop PA et al. Low-level fetal lead exposure effect on neurobehavioral development in early infancy. Pediatrics 1987; 80: 721–730.
Falcon M, Vinas P, Luna A . Placental lead and outcome of pregnancy. Toxicology 2003; 185: 59–66.
Bellinger D, Leviton A, Allred E, Rabinowitz M . Pre- and postnatal lead exposure and behavior problems in school-aged children. Environ Res 1994; 66: 12–30.
Bunn TL, Parsons PJ, Kao E, Dietert RR . Exposure to lead during critical windows of embryonic development: differential immunotoxic outcome based on stage of exposure and gender. Toxicol Sci 2001; 64: 57–66.
Han S, Pfizenmaier DH, Garcia E, Eguez ML, Ling M, Kemp FW et al. Effects of lead exposure before pregnancy and dietary calcium during pregnancy on fetal development and lead accumulation. Environ Health Perspect 2000; 108: 527–531.
Hanada T, Yoshimura A . Regulation of cytokine signaling and inflammation. Cytokine Growth Factor Rev 2002; 13: 413–421.
Baghurst PA, McMichael AJ, Vimpani GV, Robertson EF, Clark PD, Wigg NR . Determinants of blood lead concentrations of pregnant women living in Port Pirie and surrounding areas. Med J Aust 1987; 146: 69–73.
Agency for Toxic Substances and Disease Registry (ATSDR). Toxicological Profile for Lead. US Department of Health and Human Services, Public Health Service: Atlanta, GA, 1999.
Acknowledgements
This work was supported in part by cooperative agreement number: US7/CCU918557-03 from the Centers for Disease Control and Prevention.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on Journal of Perinatology website (http://www.nature.com/jp)
Supplementary information
Rights and permissions
About this article
Cite this article
Jelliffe-Pawlowski, L., Miles, S., Courtney, J. et al. Effect of magnitude and timing of maternal pregnancy blood lead (Pb) levels on birth outcomes. J Perinatol 26, 154–162 (2006). https://doi.org/10.1038/sj.jp.7211453
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211453
Keywords
This article is cited by
-
Environmental influences on child health outcomes: cohorts of individuals born very preterm
Pediatric Research (2023)
-
Birth Size Outcomes in Relation to Maternal Blood Levels of Some Essential and Toxic Elements
Biological Trace Element Research (2023)
-
Levels of non-essential trace metals and their impact on placental health: a review
Environmental Science and Pollution Research (2022)
-
The Relationship Between Heavy Metal Exposure, Trace Element Level, and Monocyte to HDL Cholesterol Ratio with Gestational Diabetes Mellitus
Biological Trace Element Research (2021)
-
Biomonitoring of Lead Exposure in Children from Two Fishing Communities at Northern Colombia
Biological Trace Element Research (2021)